
Illinois Prisons Promised Better Healthcare—Why After 7 Years Are Inmates Still Suffering?
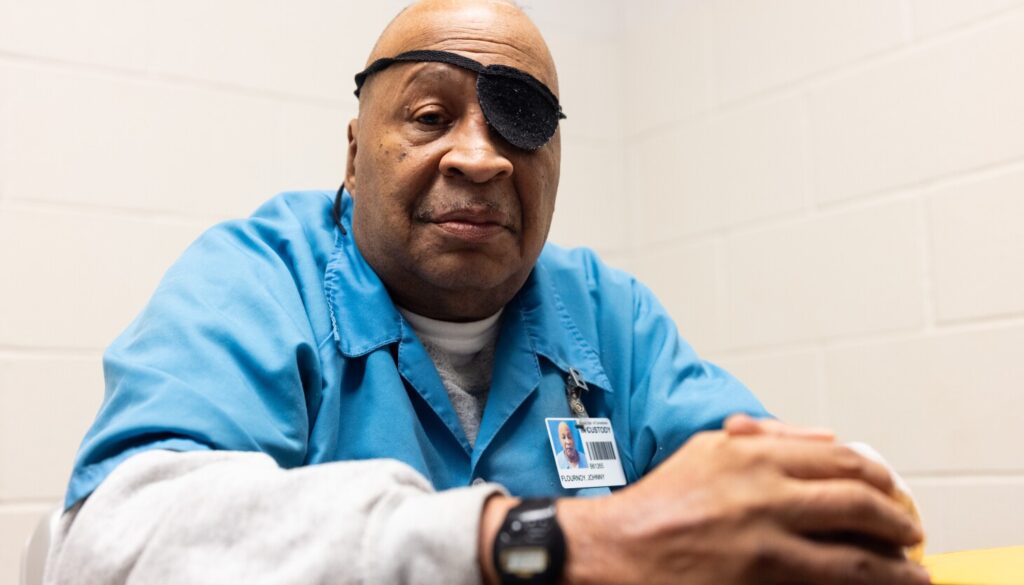
At 74 years old, Johnnie Flournoy is facing an agonizing fate: he is going blind. His vision issues began with the unsettling experience of “seeing smoke,” a symptom he first noticed while incarcerated at the Pinckneyville Correctional Center, a medium-security prison located nearly five hours south of Chicago. Flournoy has been in Illinois prisons since the early 1990s, and his struggle with vision has become emblematic of a broader crisis affecting the state’s prison healthcare system.
Diagnosed with glaucoma in 2002, Flournoy's sight continued to deteriorate over the years. Despite the condition being manageable with daily prescription eye drops—a medication available for as little as $10 for those with insurance—Flournoy often went months without receiving his medication. “I’m telling myself, I know I’m in a no-smoking institution,” he recalled, confused about his worsening eyesight. In 2007, a doctor informed him that his untreated glaucoma was wreaking havoc on his optic nerves. After suffering through five surgeries, he has now lost all vision in his left eye and fears that the same fate awaits his right.
“They let me go blind,” Flournoy lamented. “And they still ain’t doing nothing.” His attempts to secure consistent medical care have included filing grievances and even winning two settlements after suing over his vision issues. Yet, the situation remains dire, as he continues to report irregular access to necessary eye drops.
The Illinois Department of Corrections (IDOC) did not comment specifically on Flournoy’s medical history or his allegations of neglect. However, his story is not an isolated incident; it illustrates a systemic crisis within Illinois' correctional healthcare system, which has been under a consent decree since 2019, following a class-action lawsuit highlighting inadequate medical care. Reports from an independent court-appointed monitor have revealed ongoing failures in delivering appropriate medical and dental care to the state's prison population, estimated at over 30,000 inmates.
A Broken System
According to the monitor’s ninth report, several deficiencies continue to plague the IDOC:
- The department currently employs only the equivalent of 16 full-time physicians across its 29 facilities, despite being budgeted for roughly 33.
- Over the last six years, 49 physicians have resigned, contributing to dangerously low staffing levels.
- Nearly 60% of nursing positions remain vacant, and a quarter of the facilities lack a medical director.
- Most patient records are still on paper, making it difficult to track medical conditions or ensure continuity of care.
Tragically, three of the 15 deaths in custody reviewed by the monitor since the last report were attributed to preventable causes such as asthma. “People are sentenced to prison. They’re not sentenced to die from preventable diseases,” remarked Alyssa Meurer, an attorney with the Uptown People’s Law Center and a member of the legal team involved with the lawsuit that led to the consent decree.
An IDOC spokesperson asserted the department’s commitment to providing “safe, high-quality, and clinically appropriate healthcare” but failed to address a comprehensive list of questions regarding current healthcare conditions in state prisons. Legal experts, however, assert that little has changed since the consent decree was enacted. “The reality is they’ve done very little,” stated Samantha Reed, an attorney at the American Civil Liberties Union of Illinois.
One of the few areas where the IDOC has complied is in improving its written policies. Still, as Meurer pointed out, “there’s change on paper, but it has not actually effectuated any change within the facilities day to day with patient care.” This sentiment highlights a sobering truth: while the department may have made policy adjustments, the actual implementation of those policies remains scant.
Private healthcare providers like Wexford Health Sources, which previously held the contract for prison medical services, have faced scrutiny for delivering inadequate care. After the state abruptly ended its contract with Wexford last summer, it entered into an emergency agreement with Centurion Health. However, reports indicate that healthcare has not improved under the new provider, with inmates continuing to face significant lapses in care.
Flournoy’s case encapsulates the broader issue. He grapples not only with his vision loss but also with other untreated medical problems, including a hernia and heart arrhythmia. His family plays an essential role in advocating for him; his sister often contacts prison officials to secure medical attention. “He keeps telling me, ‘Just hold on. I’m coming home,’” Patricia Brown said, highlighting the family bond that fuels Flournoy’s fight.
As Flournoy navigates his diminishing sight, he remains resolute. “I’m not going to lose my mind,” he said, accepting his fate with a measure of strength. His story serves as a poignant reminder of the urgent need for reform in a system that continues to fail its most vulnerable populations.



You might also like: