
Shocking Truth: 70% of Female University Students in Bangladesh Are Ignorant About HPV Risks!
Recent research conducted among female university students in Bangladesh has unveiled concerning gaps in knowledge regarding HPV infection and its link to cervical cancer. The study, which surveyed 800 students, highlights the influence of various factors such as academic background, access to healthcare, and education on the awareness of HPV and the effectiveness of the HPV vaccine.
Findings indicate a significant relationship between students' faculty and their understanding of HPV. Students from the Biological Sciences faculty exhibited the highest level of knowledge, with 30.6% demonstrating good awareness. In contrast, only 12.8% of those from the Social Science faculty reported similar knowledge levels. Geographically, participants from Sylhet led with an impressive 88.2% exhibiting good knowledge, while those from Khulna had the lowest at just 5.7%.
Access to healthcare facilities also played a role in the students' knowledge about HPV. Female students with easy access to healthcare had a higher prevalence of good knowledge at 19.9%, compared to 12.6% among those facing difficulties. Additionally, maternal education significantly impacted awareness; participants whose mothers held a graduate degree had a knowledge rate of 23.9%, whereas those with mothers lacking formal education reported only 13.9% knowledge.
The study found a strong correlation between sexual health education and understanding HPV, with 23.4% of students who received such education demonstrating good knowledge versus only 11.0% of those who did not. Interestingly, attitudes toward premarital sex also emerged as a significant factor; 31.2% of students who were supportive of premarital sex displayed good knowledge of HPV, compared to 17.1% who opposed it.
When it comes to knowledge about the HPV vaccine, the findings were equally alarming. A significant portion of participants, 53.1%, were unsure if the HPV vaccine protects against cervical cancer. While 44.8% acknowledged its protective capabilities, knowledge about the vaccine's effectiveness against different types of HPV was lacking, with 64.7% unsure. Furthermore, 70.7% were unaware that the vaccine could protect against sexually transmitted infections, and 68.6% did not know that it is available for both men and women. Misconceptions were rampant; 88.1% erroneously believed the vaccine eliminated the need for Pap smears, and 62.4% were unaware that vaccinated individuals are not entirely free from the risk of cervical cancer in the future.
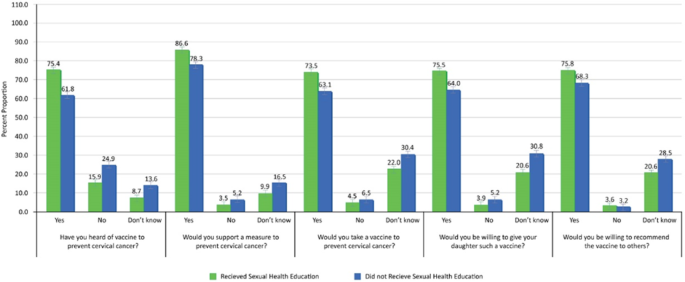
Further analysis of the data revealed that students who had received sexual health education were more aware of the HPV vaccine, demonstrating higher willingness to vaccinate themselves and recommend it to others. Among those who received sexual health education, 75.4% had heard of the vaccine compared to 61.8% of those who did not. Moreover, 86.6% of the educated group supported measures to prevent cervical cancer, and 73.5% were willing to vaccinate, while only 63.1% of those lacking education felt the same.
The study also conducted a Confirmatory Factor Analysis (CFA) to assess knowledge of HPV infection and vaccination, attitudes towards vaccination, and willingness to be vaccinated. The analysis showed that attitudes towards the vaccine had the most significant impact on the willingness to vaccinate, with a path coefficient of 0.61. Knowledge of the HPV vaccine also positively influenced attitudes (0.46), while understanding HPV infection had a negligible impact (0.07).
In terms of information sources, a concerning 22.0% of participants reported they had “never heard” of HPV. The primary sources of information included family and friends (16.6%) and social media (16.6%), while educational institutions contributed only 10.6%. Traditional media outlets and healthcare providers were cited as minimal sources of information, indicating a substantial gap in formal education about HPV.
Barriers to vaccine uptake were also identified. The most significant concern among students was regarding side effects (39.8%), followed by doubts about the vaccine’s efficacy (23.3%) and cost issues (14.8%). Other obstacles included a need for parental approval (8.1%) and general disinterest (5.6%). These findings emphasize the need for enhanced education and outreach regarding HPV and its vaccination.
Overall, the research indicates an urgent need for strengthened sexual health education programs and more accessible healthcare resources to improve awareness of HPV and cervical cancer prevention strategies among female university students in Bangladesh. The gaps in knowledge and misconceptions surrounding the HPV vaccine highlight the critical need for clear, factual information to empower young women in making informed health decisions.





You might also like: