
You Won't Believe How New Research is Shocking Alzheimer's and Parkinson's Patients – Discover the Hidden Truth!
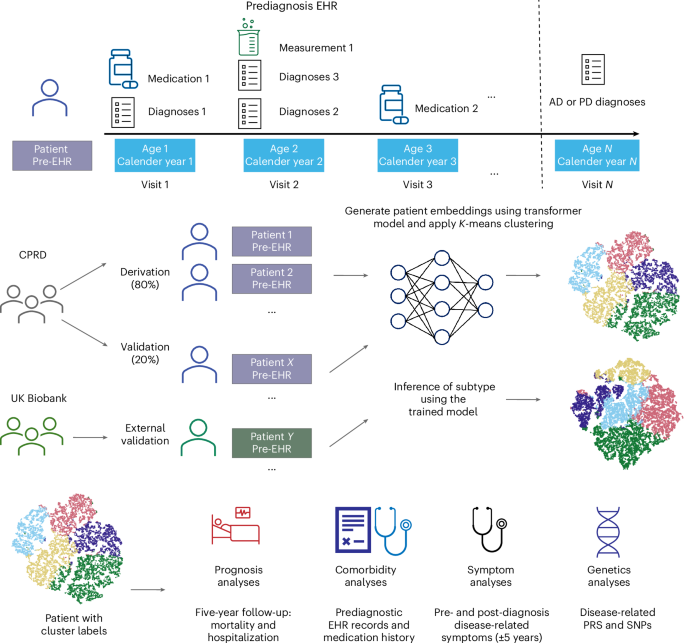
A recent study utilizing data from the Clinical Practice Research Datalink (CPRD) Aurum and the UK Biobank sheds light on the complexities of Alzheimer’s disease (AD) and Parkinson’s disease (PD), revealing five distinct subtypes for each condition. This innovative research aims to enhance the understanding of these neurodegenerative diseases, which affect millions of Americans and their families.
The study, which analyzed extensive electronic health record (EHR) data covering approximately 20% of the UK population, identified a total of 113,545 patients with AD and 45,825 patients with PD who met the inclusion criteria. The mean age at diagnosis for AD was 82.1 years in the CPRD cohort and 74.4 years in the UK Biobank cohort. Females constituted 63.8% of the CPRD group and 52.1% of the UK Biobank group. Notably, only 0.2% of AD patients in CPRD were between 40 and 50 years old, while a significant 64.9% were over 80 years old.
For PD, the mean diagnosis age was slightly younger at 77.8 years for CPRD participants and 70.6 years for those in the UK Biobank. The gender distribution showed that women comprised 40.6% of the CPRD group and 37.1% of the UK Biobank group. Again, the younger demographic was limited, with only 0.93% of patients aged 40-50 in CPRD.
In this study, longitudinal prediagnostic EHRs were employed to characterize AD and PD subtypes. Using advanced machine learning techniques, including a transformer model for data representation and K-means clustering, researchers identified five distinct clusters for each condition based on prognosis, comorbidities, symptoms, and genetic factors. The clusters revealed significant differences in mortality and hospitalization rates; for instance, AD patients in cluster 1 had a 5-year mortality rate of approximately 55%, while those in cluster 5 faced rates as high as 70%. Similar trends were observed in PD, with cluster 1 showing the lowest mortality and hospitalization rates at about 50% and 65%, respectively.
Understanding the Subtypes
The five subtypes identified in AD encompass a range of characteristics. Cluster 1 represents a classic late-onset presentation, accounting for 27.7% of CPRD patients. This cluster predominantly features females. Cluster 2 outlines vascular-related patterns, while cluster 3 highlights neuropsychiatric dominance. Cluster 4 is characterized by metabolic–inflammatory profiles, and cluster 5 identifies a sensorimotor pattern. In the PD cohort, cluster 1 also stands out as the most prevalent, with 28.8% of patients exhibiting classic genetic PD traits. Other clusters in PD reflect varying characteristics, such as vascular-associated types and severe neuropsychiatric forms.
Analyzing these clusters reveals a nuanced understanding of comorbidities. For instance, cluster 2 in AD was predominantly defined by essential hypertension affecting 94% of patients, while cluster 3 exhibited high prevalence rates of hypothyroidism (52%) and respiratory diseases. Cluster 4 stood out with 97% diabetes prevalence, while cluster 5 was characterized by cardiovascular diseases, including a 20% prevalence of late-stage syphilis.
Furthermore, symptom trajectories were meticulously tracked over 10 years, providing insight into early signals of disease progression. AD clusters showed that cluster 3 had the highest incidence of depression and anxiety, with subsequent cognitive decline evident in Mini-Mental State Examination (MMSE) scores. Similarly, in PD cohorts, cluster 3 exhibited the most severe symptoms, including earlier tremor manifestations and increased anxiety and depression.
Genetic analysis further illuminated the distinct profiles of these clusters. Using polygenic risk scores (PRS), researchers found that all AD clusters had significantly higher PRS scores than controls, with cluster 4 notably having a lower score, suggesting a potential protective factor. For PD, clusters displayed significant genetic variability, notably with cluster 2 showing increased risk for conditions such as hypertension and stroke.
This comprehensive study underscores the importance of understanding the heterogeneous nature of neurodegenerative diseases. As the American population ages, the prevalence of AD and PD is expected to rise, making it critical for healthcare systems to adapt. The findings could help tailor more effective, individualized treatment plans and interventions, ultimately improving patient outcomes. As research continues to evolve, understanding these subtypes will be pivotal in addressing the complexities of AD and PD, fostering hope for patients and their families.




You might also like: