
What Shocking Vaccine Secrets Were Uncovered in September 2025? You Won't Believe the Consequences!
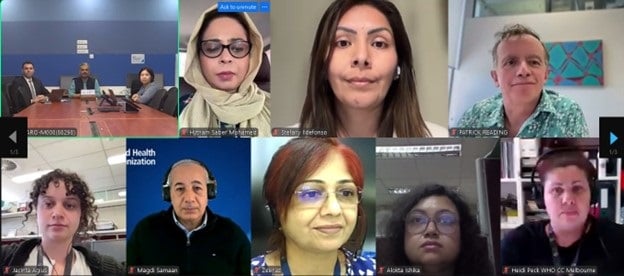
On March 30, 2026, the World Health Organization's Regional Office for South-East Asia (WHO SEARO) convened a pivotal regional webinar. This event gathered experts from the WHO’s Global Influenza Programme (GIP), various WHO Country Offices, National Influenza Centres (NICs) within SEAR Member States, and WHO Collaborating Centres for Influenza Research and Reference based in Melbourne and Tokyo. The primary focus of this session was to review recent developments in influenza surveillance, virological trends, and the global vaccine composition determination process, particularly concerning the upcoming 2026 Southern Hemisphere vaccine and the 2026–2027 Northern Hemisphere vaccine.
Dr. Nilesh Buddha, Regional Emergency Director and Acting Director of Programme Management at WHO SEARO, opened the session by emphasizing the increasing complexity of the environment in which influenza surveillance systems operate. These challenges include financial constraints and competing public health priorities. Despite these obstacles, countries in the region have demonstrated a strong commitment to performance on key surveillance indicators, maintaining regular and consistent reporting. This commitment is essential for early detection of influenza activity, supporting global risk assessments, and preparing for seasonal, zoonotic, and potential pandemic influenza.
During the discussion, it became clear that influenza surveillance is not merely about data collection; it is a systematic process generating ongoing information to guide public health actions on national, regional, and global levels. By integrating genetic, antigenic, and serological data, countries contribute critical evidence that informs vaccine composition decisions and global risk assessments. Member States are active contributors to this evidence generation within a highly interconnected Global Influenza Surveillance and Response System.
The recent surveillance data illustrated clear and consistent seasonal influenza patterns across the region. Most countries met the WHO-recommended testing threshold of at least 50 samples per week at the national level, although some variability among countries was noted. National Influenza Centres generally exhibited high diagnostic performance, validated through external quality assurance mechanisms. However, a systematic and continuous reporting of unsubtyped influenza viruses, particularly influenza A, remains an area in need of strengthening.
Virological analysis revealed the diverse circulation of influenza viruses, including A(H3), A(H1N1), and influenza B, with significant variation observed across countries. The robust influenza surveillance systems in the region also proved effective in detecting zoonotic spillover events, with human infections caused by avian influenza A(H5N1) reported in Bangladesh and India. The emergence of new variants, such as the recently detected H3 clade K, highlights the continual need for monitoring through influenza surveillance, genomic sequencing of representative samples, and timely public reporting to support regional and global actions.
The webinar also underscored the importance of rapid reporting of non-seasonal influenza subtypes under the International Health Regulations (IHR). Countries are required to notify WHO within 24 hours of any event that may pose a public health risk, which includes human infections from new influenza subtypes. A significant portion of signals is detected through event-based surveillance systems that utilize media monitoring and informal sources, emphasizing the necessity for rapid verification, analysis, and timely reporting to facilitate effective public health responses.
Advancements in data systems were also discussed, particularly highlighting the Public Health Intelligence Dashboard. While the Influenza Programme maintains its dashboards under the Global Influenza Strategy (2019–2030), this new dashboard integrates multi-disease data, including influenza, into a single platform to support emergency response decision-making. It enables real-time visualization and country-level analysis, enhancing accessibility to integrated data and fostering timely, informed decision-making across health systems.
A central theme during the discussions was the critical role of timely and representative virus sharing. Samples submitted by National Influenza Centres to WHO Collaborating Centres undergo detailed genetic, antigenic, and serological analyses that are foundational for understanding circulating influenza viruses. Dr. Patrick Reading, Director of the Victorian Infectious Diseases Reference Laboratory (VIDRL) in Melbourne, emphasized that the value of virus samples is highly dependent on their timeliness and representativeness.
Dr. Magdi Samaan from WHO Headquarters (GIP) illuminated how global data is translated into vaccine recommendations. He noted that these decisions are based on the integration of surveillance data, genomic sequencing, and laboratory analyses, ensuring recommendations are grounded in the most comprehensive and up-to-date evidence available. Thus, timely and high-quality data inputs from countries are essential for accurate vaccine strain selection, ultimately supporting effective population protection.
The experience of Myanmar was presented by Dr. Yee Mon Mya, showcasing that influenza surveillance can be maintained even in challenging operational environments. Despite facing conflict, logistical constraints, and limited human resources, Myanmar has successfully sustained surveillance by implementing adaptive strategies, including expanding sentinel sites and employing flexible implementation approaches.
The webinar concluded by outlining key priorities for strengthening the regional influenza surveillance systems. These include enhancing consistency in testing, particularly for influenza subtyping and reporting, improving the completeness of laboratory data, and ensuring timely and representative virus sharing with WHO. As the global health landscape continues to evolve, the insights and commitments made during this session will be crucial for enhancing preparedness and responsiveness to influenza threats across the region.



You might also like: