Scientists Just Unveiled a Controversial Fentanyl Vaccine—Is This the Key to Ending the Epidemic?
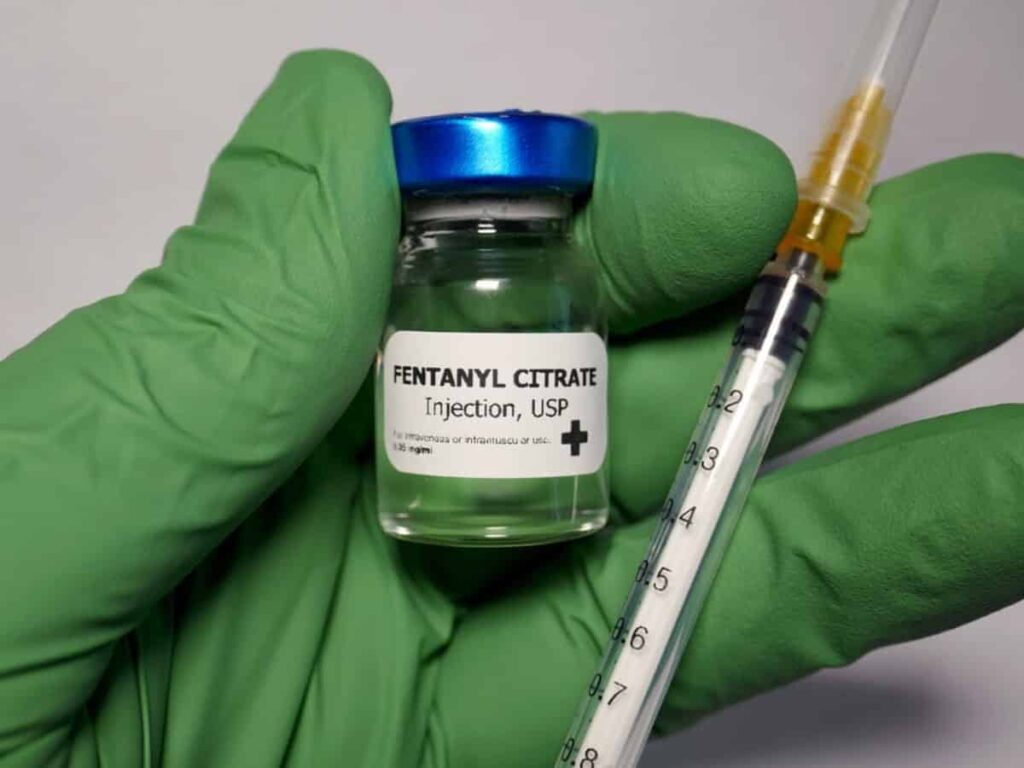
In the ongoing battle against opioid overdoses, a new frontier is emerging: a potential fentanyl vaccine designed to intervene before the drug can wreak havoc on the body. Fentanyl, a synthetic opioid that can be fatal in doses as small as a few grains of salt, is responsible for nearly 70% of overdose deaths in the United States. As communities grapple with this crisis, a biotech company named ARMR Sciences is taking bold steps to combat the epidemic by developing a vaccine that aims to prevent fentanyl from ever reaching the brain.
Currently, the most widely available treatment for an opioid overdose is Naloxone, which acts as a quick reversal agent but only after the overdose has already begun. In cities across the country, Naloxone is as common as fire extinguishers, with its presence symbolizing the urgent need for intervention. However, as Collin Gage, ARMR’s cofounder and chief executive, noted in an interview with Wired, "everything that exists is reactionary." His vision is for a preemptive solution to the fentanyl crisis.
The Fentanyl Vaccine
ARMR Sciences plans to launch its first human trial for the fentanyl vaccine in early 2026 at the Centre for Human Drug Research in Leiden, Netherlands. This trial will involve approximately 40 healthy adults. The concept of a vaccine targeting synthetic opioids isn't entirely new; researchers have been exploring such options since the 1970s. However, earlier attempts at developing opioid vaccines proved ineffective, leading to a decline in interest until the modern overdose crisis reignited the discussion.
What makes ARMR’s approach unique is the way it aims to train the immune system to recognize fentanyl. Traditional vaccines target viruses or bacteria, but fentanyl is so minuscule that it often goes unnoticed by the immune system. To tackle this, the ARMR vaccine links a fentanyl-like fragment to a larger carrier protein, CRM197, a deactivated diphtheria toxin already used in approved vaccines. An adjuvant derived from E. coli toxins further enhances the immune response.
In preliminary trials conducted on rats at the University of Houston in collaboration with Tulane University, the vaccine demonstrated impressive results, blocking 92% to 98% of fentanyl from entering the brain. The effectiveness lasted for around 20 weeks, raising hopes for similar outcomes in humans.
The upcoming human trial will unfold in stages, with initial focus on safety and monitoring for side effects. After establishing safety, a small group of participants will receive low doses of fentanyl under strict medical supervision to assess how effectively the vaccine blocks its effects. Gage describes the vaccine as a "suit of armor," emphasizing its potential to change the paradigm of overdose treatment by removing the necessity for immediate access to treatment in emergency situations.
However, challenges remain. The finite nature of produced antibodies means that a high enough dose of fentanyl could potentially overwhelm the body’s defenses. Dr. Sharon Levy, an addiction specialist at Boston Children’s Hospital and an adviser to ARMR, cautioned, “There’s only going to be so many antibodies.” Additionally, there are concerns regarding its implications for pain management, as fentanyl plays a crucial role in anesthesia and emergency medicine. Researchers assure that animal studies indicate the vaccine would not interfere with other opioids, such as morphine or methadone.
Interest in the vaccine appears to be strong, particularly among at-risk populations such as teenagers and young adults who may encounter fentanyl unknowingly. Surveys indicate that individuals in treatment for opioid use disorder also view the vaccine as a beneficial preventative measure. Other scientists are exploring complementary strategies, including monoclonal antibody treatments that could provide about a month of protection. As noted by Marco Pravetoni, who is developing such an approach, “We think a month of protection is pretty good in terms of providing a safety net.”
It’s essential to recognize that while the potential vaccine may provide a new layer of defense, it is not a complete solution. No single intervention can eliminate addiction or dismantle the illicit drug market. Given the gravity of the opioid crisis that has impacted nearly half of American families, Gage’s personal motivation reflects a broader reality: “I had two close childhood friends who passed away from fentanyl overdose. Neither of them were seeking it out.”
As ARMR’s vaccine approaches clinical testing, it holds the promise of a future where overdose prevention may not rely solely on emergency responses but on long-term immunity against fentanyl. In a landscape where every day lost to opioid addiction can have devastating consequences, this new line of defense could be a game changer in the fight against the opioid crisis.




You might also like: